“Is there something we are missing?”
Usually, I hear this question during consultations when pregnancy is delayed. Behind these, there is confusion, quiet silence and worry. Initially, male infertility is not considered in many cases.
Because many people think infertility is only a woman’s struggle, but the truth is that male infertility is just as common.
I often see how this misunderstanding creates significant stress for men, making it harder for them to speak openly.
As a doctor, I want to shift this perspective by helping couples understand the male infertility meaning. It is a medical condition, like any other, and there is no reason to feel ashamed.
Once we identify the cause, we can guide you toward the right treatment and move forward together with clarity and hope.
What Is Male Infertility?
Male infertility means a male partner is not able to have a biological child with his female partner.
In our clinical experience, we see that some male factors, such as sperm issues, male reproductive health issues or lifestyle, are responsible for male infertility.
According to the All India Institute of Medical Sciences, New Delhi (AIIMS), around 10-15% couples are facing infertility in India. Among these, around 40-50% infertility issues are related to male factors.
This data shows male infertility plays a big part in India’s overall infertility rates.
Signs and Symptoms of Male Infertility
Unlike women fertlity, men have no signs or symptoms that indicate any underlying condition. In fact, you may not realise there is an issue until pregnancy does not happen with regular attempts.
So, how do you recognise the signs of infertility in men?
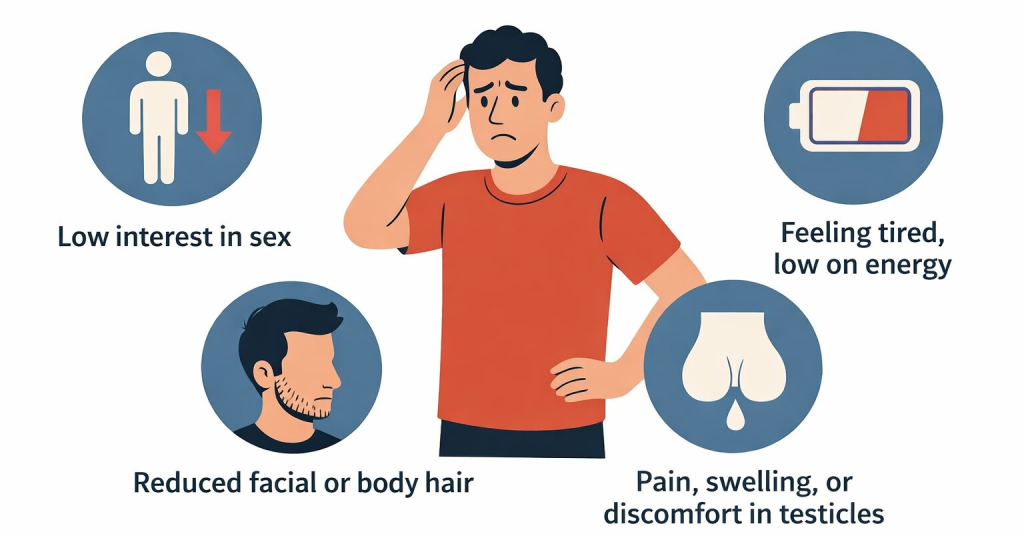
In some cases, you may notice some changes, especially symptoms of low sperm count, such as:
- Changes in sexual function, including low interest in sex or issues like early or delayed ejaculation
- Reduced facial or body hair, which may indicate a hormonal imbalance
- Pain, swelling, or discomfort in the testicular area
- Feeling unusually tired, low on energy, or experiencing mood changes, due to low testosterone levels
So, if you notice these signs, the next question is: what is causing them? Let’s understand the possible reasons behind male infertility.
Common Causes of Male Infertility
We see that the most common cause of male infertility is related to problems with sperm. A study published in The National Medical Journal of India also highlights that around 40% of men had abnormal semen parameters.
Another important cause of male infertility is as follows:
1. Sperm-related issues:
- Low sperm count (oligospermia): Fewer sperm reduce the chances of fertilization.
- Zero sperm count (azoospermia): No sperm are present in the semen.
- Poor sperm motility: Sperm struggle to move effectively toward the egg.
- Abnormal sperm shape: Irregularly shaped sperm cannot fertilize properly.
2. Medical conditions:
- Varicocele: Swollen veins in the scrotum, which interfere with sperm production and quality. This is the most common reversible cause.
- Infections: Reproductive tract infections that damage sperm or block their movement.
- Other medical conditions: Diabetes, thyroid issues, genetic disorders and cystic fibrosis can affect sperm production.
3. Hormonal imbalance:
- Low testosterone levels: Reduce sperm production and sexual function.
- Other hormone imbalance: Can arise from issues in the testicles or from imbalances in hormone-regulating glands such as the hypothalamus, pituitary, or adrenal glands.
4. Lifestyle factors:
- Smoking & alcohol: Lower sperm health and quality.
- Obesity: It is linked to reduced fertility and hormonal changes.
- Stress: It interferes with hormone balance and sperm production.
Understanding these causes is an important step, but identifying the exact cause in your case requires a thorough diagnosis. If you are unsure what to expect, reading about what happens during your first visit to a fertility clinic can help you feel more prepared.
How Is Male Infertility Diagnosed?
Every patient’s journey is unique, so we focus on understanding your condition first before deciding the next steps.
For this, we follow a simple step-by-step approach:
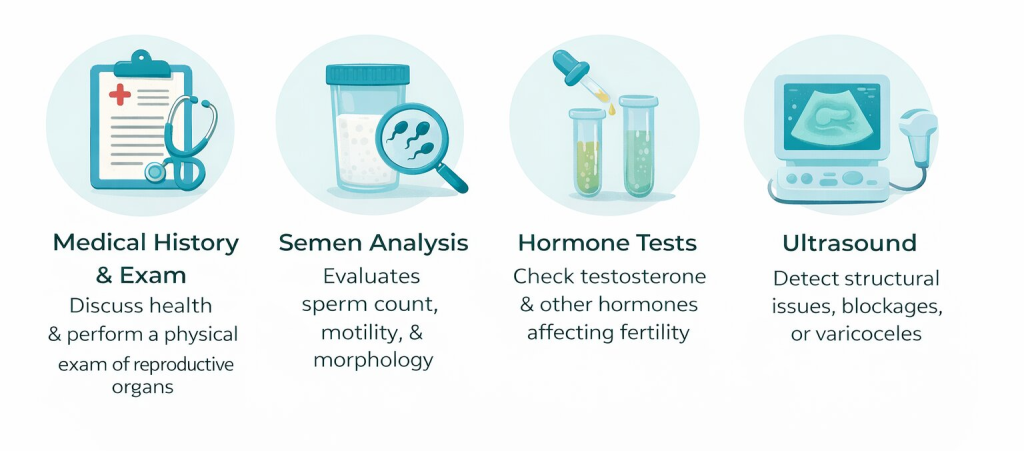
- Medical history & exam: We will start by discussing your health and performing a physical exam of your reproductive organs.
- Semen analysis: This is one of the most important tests, during which we evaluate sperm count, motility, and morphology.
- Hormone tests: We check testosterone and other hormones that control your fertility.
- Ultrasound: We sometimes use it to detect structural problems, blockages, or varicoceles.
With these results, we can guide the right treatment and support your journey. So, what treatment options are available for male infertility? Let’s take a look.
Available Treatment Options for Male Infertility
There are various treatment options for male infertility. We plan personalized treatment based on the underlying cause of each patient, whether it is medical, surgical, or assisted techniques.
Let’s understand these options in a simple way:
| Category | Treatment | Simple Explanation |
| Medical Treatment | Medications for infections | If an infection is affecting your sperm health, antibiotics can clear it up and improve your fertility. |
| Hormone therapy | When your hormones are out of balance, medications can help sperm release properly. | |
| Surgical Treatment | Varicocele treatment | Surgery fixes swollen veins in the testicles. |
| Correction of blocked ducts | If sperm are blocked from flowing, surgery can open the ducts and restore normal movement. | |
| Assisted Reproductive Techniques | IUI (Intrauterine Insemination) | Healthy sperm are placed directly into the uterus, increasing their chances of meeting the egg. |
| IVF (In Vitro Fertilization)+ ICSI (Intracytoplasmic Sperm Injection) | IVF combines eggs and sperm in a lab. ICSI goes one step further, placing a single sperm inside the egg to help fertilization. |
Together, these treatments open doors to new beginnings.
What Is TESA (Testicular Sperm Aspiration)?
In some men, especially those with very low or zero sperm count (azoospermia), sperm may still be produced inside the testicles but not present in the semen.
In such cases, we can use a simple procedure called TESA (Testicular Sperm Aspiration).
TESA is a minimally invasive technique where we collect sperm directly from the testicles using a fine needle. The procedure is usually quick, performed under local anesthesia, and does not require major surgery.
When do we recommend TESA?
We may suggest TESA in situations like:
- Zero sperm count (azoospermia)
- Blockage in sperm transport
- Previous vasectomy or failed reversal
- When sperm is not found in semen analysis
How does TESA help in pregnancy?
The sperm retrieved through TESA is not used for natural conception. Instead, it is combined with advanced fertility treatments like IVF with ICSI, where a single healthy sperm is injected directly into the egg.
This approach gives many couples a real chance of pregnancy, even in cases where it once seemed difficult.
Is TESA safe?
TESA is generally a safe and low-risk procedure. Most patients can go home the same day and resume normal activities shortly after. Mild discomfort or swelling may occur but usually settles quickly.
Can Male Infertility Be Cured?
Male infertility is not always curable, but it can be treated based on the cause. If you have any infections or hormone problems often clear up with the right care. Better lifestyle habits can also improve your health and boost fertility results.
But many of our patients have questions: Can a low sperm count be cured? We gently tell them that, in many cases, low sperm count can be effectively managed with a combination of medical care and lifestyle changes.
If you have not conceive through naturally, we advise you to consider advanced assisted reproductive techniques that offer effective solutions. For couples exploring these options, understanding how IVF works as a process can be a helpful starting point before your consultation.
Tips to Improve Male Fertility Naturally

Have you ever considered how to increase fertility in men? Yes, you can, and it starts with a simple and healthy lifestyle.
- Include food in your diet that is rich in zinc, antioxidants, and vitamins to boost your sperm health.
- Exercise regularly and maintain a healthy weight to keep your hormones balanced.
- Quit smoking and limit alcohol to protect your sperm from damage.
- Manage stress through relaxation practices such as yoga or meditation.
- Stay hydrated and get enough sleep to support your natural sperm production.
- Take fresh, whole foods over processed ones for better overall fertility health.
Advanced Fertility Solutions and Personalized Care in Palanpur

Male infertility can often be improved with timely care, whether through medicines, surgery, or advanced techniques. With expert guidance, many couples achieve their dream of parenthood. At Kalyan Women’s Hospital & IVF Center in Palanpur, under the guidance of Dr Rahul Patel, patients receive expert guidance, advanced diagnostics, and compassionate care. Helps couples move forward with confidence on their journey to parenthood.
If you have been trying to conceive and have questions, you can book an appointment with our team to discuss your concerns in a private and supportive setting.
FAQs
Treatment depends on the cause. Lifestyle changes and medication are usually the first steps. If a varicocele is found, surgery is often recommended as it is one of the most reversible causes. For couples who have not conceived through other means, assisted techniques like IUI, IVF, or ICSI are considered.
Not always, but it can often be treated or managed effectively. Infections and hormonal imbalances frequently respond well to medication. Structural problems may be corrected surgically. Even in complex cases, techniques like ICSI allow fertilization using very few sperm, giving many couples a realistic path to parenthood.
Male infertility rarely has obvious symptoms. The most common sign is simply not achieving pregnancy after regular attempts. In some cases, changes in sexual function, reduced body or facial hair, pain or swelling around the testicles, or low energy may point to an underlying issue worth investigating.
Yes, in many cases. A low sperm count reduces the probability of natural conception but does not make it impossible. With medical support, lifestyle improvements, or assisted reproductive techniques, many men with low sperm count have gone on to father children.
Nutrients that support sperm health include zinc, vitamin C, vitamin E, vitamin D, CoQ10, L-carnitine, selenium, and omega-3 fatty acids. These help protect sperm from oxidative damage and support motility. It is advisable to speak with a doctor before starting any supplements, as dosage and individual needs vary.
Diagnosis typically starts with a medical history review and physical examination, followed by a semen analysis to assess sperm count, motility, and shape. Hormone tests and an ultrasound may also be recommended depending on initial findings.

